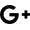In the world of medical supplies, terms like sterile and non-sterile are used every day. But for a procurement manager at a major hospital or a distributor stocking a warehouse, the difference between sterile and non-sterile supplies is more than just terminology—it’s a critical distinction that impacts patient safety, clinical outcomes, and budget allocation. Choosing the wrong type of dressing for a wound can lead to serious complications. As a manufacturer of medical consumables with a global client base, I, Allen, understand the questions and concerns that arise when sourcing these essential items. This article is designed to provide a clear, comprehensive guide to understanding sterile and non-sterile dressings, helping you make informed decisions to ensure you provide the best care possible.
What Exactly Defines a Sterile Dressing?
A sterile dressing is a wound covering that is guaranteed to be completely free of microorganisms. This doesn’t just mean it’s clean; it means it is entirely free from all living germs, including bacteria and viruses. To achieve this state, the dressing undergoes a rigorous sterilization process at the manufacturing facility. This process, which can involve methods like radiation, ethylene oxide gas, or high-pressure steam, is designed to kill every last microorganism on the dressing.
After the sterilisation process, sterile dressings come individually wrapped in packaging that is designed to act as a barrier against any outside contaminant. The integrity of this packaging is crucial. Once it is opened, the dressing is no longer considered sterile. This level of cleanliness is essential for any medical procedure where the skin is broken, as it helps to reduce the risk of infection in a vulnerable wound. A sterile dressing is a foundational tool in proper wound care.
And What is a Non-Sterile Dressing?
A non-sterile dressing, on the other hand, is a dressing that is considered clean but has not undergone a special sterilization process to be made completely free from germs. These dressings are manufactured in a clean environment, but they are not guaranteed to be free of every single microscopic germ. They are often packaged together in bulk rather than being individually wrapped. A non-sterile dressing is perfectly safe and effective for a variety of medical applications where the risk of introducing infection is very low.
The primary use for a non-sterile dressing is on intact skin or for closed wounds. For example, they are ideal for providing cushioning over a bruise, supporting a sprain, or as a secondary dressing layered on top of a primary sterile dressing to add bulk and absorbency. Because the manufacturing process is less complex and the packaging is simpler, a non-sterile dressing is generally cheaper than sterile ones, making it a cost-effective choice for appropriate situations.

What are the Key Differences Between Sterile and Non-Sterile Gauze?
Gauze is one of the most common types of dressing material, with a use dating back centuries. As one of the oldest medical supplies, it’s available in both sterile and non-sterile gauze formats. Understanding the differences between sterile and non-sterile gauze is fundamental for first aid and medical professionals. Let’s break down the key differences in a simple table.
| Feature | Sterile Gauze Dressing | Non-Sterile Gauze Dressing |
|---|---|---|
| Condition | Completely free of microorganisms. | Clean, but not guaranteed to be free of all germs. |
| Primary Use | Direct application on open wounds, cuts, burns, and surgical sites. | Closed wounds like bruises, padding, support, or as a secondary dressing. |
| Packaging | Individually wrapped to maintain sterility. | Often packaged in bulk (e.g., rolls or multi-packs). |
| Cost | More expensive due to the sterilisation process and packaging. | Generally cheaper and more economical for bulk use. |
| Infection Risk | Lowers the risk of infection when used correctly on an open wound. | Non-sterile dressings may introduce bacteria into the wound if used on broken skin. |
This sterile vs non-sterile distinction is the most important factor when choosing the right dressing for any wound.
Why Must You Use a Sterile Dressing on Open Wounds?
Using a sterile dressing on open wounds is a non-negotiable rule in medicine. When the skin—our body’s natural barrier against germs—is broken by a cut, abrasion, or surgical cuts, it creates a direct pathway for bacteria and other microorganisms to enter the body. This can lead to a serious infection after the wound has been sustained. An infection not only delays the healing process but can also complicate the injury and lead to more severe health issues.
A non-sterile dressing, even if it looks clean to the naked eye, can carry a multitude of invisible microorganisms. Placing this type of dressing directly onto an open wound is a surefire way to introduce bacteria into the wound. A sterile dressing, on the other hand, provides a clean and safe barrier. It protects the exposed tissue from environmental contaminants and helps create an optimal environment for the body to begin its natural healing process. For everything from minor cuts to a major incision, a sterile dressing is the only safe choice to reduce infection.
When is it Appropriate to Use a Non-Sterile Dressing?
While a non-sterile dressing is unsafe for open wounds, it has many important and appropriate uses in medical care where the infection risk is minimal. These dressings are generally the workhorses for situations involving intact skin. For example, a non-sterile gauze roll is perfect for securing a splint or providing light compression over a sprain. It can be used to provide padding under a cast to prevent chafing, or to cushion a simple bruise.
A non-sterile dressing can also function as an effective secondary dressing. In this role, it is placed on top of a primary sterile dressing that is already covering the wound. Here, its job is to add extra absorption for a heavily draining wound or to help hold the primary dressing in place. Because it does not come into direct contact with the open wound, its lack of sterility is not a concern. This is a common practice in clinical settings to manage wounds cost-effectively without compromising patient safety.
Can You Sterilise Non-Sterile Dressings at a Clinic?
This is a question that sometimes comes up in an effort to save costs: can you just buy a cheaper non-sterile dressing and sterilize it yourself? The short answer is that this is highly discouraged and often unsafe. The sterilization process used by manufacturers is a highly controlled, validated procedure that is difficult, if not impossible, to replicate reliably in a typical clinic or first aid setting.
Methods like boiling or using an alcohol-based disinfectant are not true sterilization—they are forms of disinfection. Disinfect means to reduce the number of germs, while sterilize means to eliminate all of them. An autoclave (a steam sterilizer) can sterilize equipment, but the packaging is key. Without the proper medical-grade packaging to place the dressing in before autoclaving, you cannot maintain sterility once it’s removed. Attempting to sterilise non-sterile dressings yourself introduces a significant risk of incomplete sterilization, which can lead to dangerous potential infections. It is always safer to use a commercially prepared sterile dressing.

How Does Packaging Help Maintain Sterility?
The packaging of a sterile dressing is just as important as the sterilisation process itself. A sterile dressing is useless if its sterility is compromised before it reaches the wound. That’s why sterile dressings come sealed in durable, individual pouches. This packaging is specifically designed to be a fortress against microorganisms. It prevents any germ from the outside environment from reaching the gauze inside.
When preparing to apply a sterile dressing, it is crucial to inspect this packaging first. If the wrapper is torn, punctured, or has been wet, you must assume the dressing is no longer sterile and discard it. When opening the package, care must be taken to not touch the sterile gauze itself. By peeling back the wrapper and allowing the dressing to fall onto a clean surface or handling it only by the very edges, you can ensure the dressing remains sterile until it is placed on the wound. This meticulous attention to handling is a fundamental part of proper wound care.
Choosing Between Sterile and Non-Sterile: A Procurement Perspective
For a procurement professional, the choice between sterile and non-sterile wound dressings is a daily balancing act of clinical need, safety, and budget. The right choice is entirely dependent on the intended use within your facility. A hospital will need a large inventory of both sterile and non-sterile dressings. Sterile gauze, like these sterile absorbent gauze pads, is an absolute necessity for the operating room, the emergency department, and for dressing any post-surgical wound.
At the same time, stocking bulk non-sterile dressing rolls and pads for tasks like orthopedic padding, secondary dressing layers, and general cleaning is a smart, cost-effective strategy. The key is clear education and protocol for clinical staff on when to use each type. Sourcing high-quality versions of both sterile and non-sterile gauze from a reliable supplier ensures that you have the right tool for every job, maximizing patient safety while managing costs efficiently. Choosing between sterile and non-sterile dressings is essential for good inventory management.

What to Look for in a Supplier of Sterile and Non-Sterile Dressings
When sourcing wound dressings, the reliability of your supplier is paramount. Whether you are buying a sterile dressing or a non-sterile dressing, you need to trust the quality of the product and the integrity of the manufacturing process. Look for a manufacturer with robust quality control certifications, such as ISO 13485 and CE marking. This demonstrates a commitment to meeting international medical device standards.
A good supplier should provide clear, transparent product information, including materials used, the sterilization method for sterile products, and accurate expiration dates. Their packaging should be durable and clearly labeled. As a manufacturer, we understand that our clients depend on this consistency. Whether it’s a disposable medical gauze bandage roll or a simple gauze swab, the quality must be unwavering. A strong partnership with your supplier is the best way to ensure you consistently receive safe and effective wound care products.
Emergency First Aid: Is a Non-Sterile Dressing Better Than Nothing?
In a true emergency situation outside of a clinical setting, the ideal supplies may not be available. What if you only have a non-sterile dressing but need to cover an open wound? In this scenario, the priority is to stop the bleeding and offer some protection from gross contamination. A clean non-sterile dressing is almost always better than using a dirty rag or leaving the wound completely exposed.
While there is still an infection risk, a clean non-sterile dressing is the lesser of two evils in a life-or-death emergency. The goal in first aid is to stabilize the situation until professional medical help can be reached. Once the person is in a proper medical facility, the wound will be thoroughly cleaned and a proper sterile dressing will be applied. So, while sterile is always the standard of care, a clean non-sterile dressing can be a temporary, necessary measure in an urgent first aid scenario.
Key Takeaways
- Sterile Means Germ-Free: A sterile dressing has undergone a process to eliminate all microorganisms and is essential for use on open wounds.
- Non-Sterile Means Clean: A non-sterile dressing is clean but not germ-free. It is safe for use on intact skin or for closed wounds.
- Application is Key: The primary difference between sterile and non-sterile is their application. Never place a non-sterile dressing directly on a broken wound.
- Packaging Protects: For a sterile dressing, the individual, sealed packaging is crucial to maintain sterility. If it’s damaged, the dressing is compromised.
- Do Not Self-Sterilize: Attempting to sterilise non-sterile dressings in a clinic is unreliable and risky. Always use commercially prepared sterile products for open wounds.
- Stock Both: A well-equipped medical facility needs a supply of both sterile and non-sterile dressings to provide comprehensive and cost-effective wound care.
Post time: Nov-11-2025